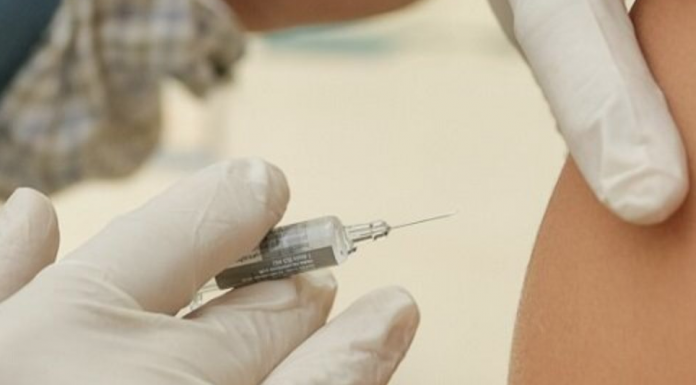
Mayo Clinic – Vaccines to prevent the coronavirus disease 2019 (COVID-19) are perhaps the best hope for ending the pandemic.
But as the U.S. Food and Drug Administration (FDA) begins authorizing emergency use of COVID-19 vaccines, you likely have questions.
Find out about the benefits of the COVID-19 vaccines, how they work, the possible side effects and the importance of continuing to take infection prevention steps.
What are the benefits of getting a COVID-19 vaccine?
COVID-19 can cause severe medical complications and lead to death in some people. There is no way to know how COVID-19 will affect you. If you get COVID-19, you could spread the disease to family, friends and others around you.
Getting a COVID-19 vaccine can help protect you by creating an antibody response in your body without your having to become sick with COVID-19.
A COVID-19 vaccine might prevent you from getting COVID-19. Or, if you get COVID-19, the vaccine might keep you from becoming seriously ill or from developing serious complications.
Getting vaccinated also might help protect people around you from COVID-19, particularly people at increased risk of severe illness from COVID-19.
What COVID-19 vaccines have been approved and how do they work?
Currently, several COVID-19 vaccines are in clinical trials. The FDA will review the results of these trials before approving COVID-19 vaccines for use.
But because there is an urgent need for COVID-19 vaccines and the FDA’s vaccine approval process can take months to years, the FDA will first be giving emergency use authorization to COVID-19 vaccines based on less data than is normally required. The data must show that the vaccines are safe and effective before the FDA can give emergency use authorization.
Pfizer/BioNTech vaccine
The FDA has given emergency use authorization to the Pfizer/BioNTech COVID-19 vaccine. Data has shown that the vaccine starts working soon after the first dose and has an efficacy rate of 95% seven days after the second dose.
This means that about 95% of people who get the vaccine are protected from becoming seriously ill with the virus. This vaccine is for people age 16 and older. It requires two injections given 21 days apart.
Moderna vaccine
The FDA has given emergency use authorization to the Moderna COVID-19 vaccine. Data has shown that the vaccine has an efficacy rate of 94.1%. This vaccine is for people age 18 and older. This vaccine requires two injections given 28 days apart.
Both the Pfizer/BioNTech and the Moderna COVID-19 vaccines use messenger RNA (mRNA). Coronaviruses have a spike-like structure on their surface called an S protein. COVID-19 mRNA vaccines give cells instructions for how to make a harmless piece of an S protein.
After vaccination, cells begin making the protein pieces and displaying them on cell surfaces. Your immune system will recognize that the protein doesn’t belong there and begin building an immune response and making antibodies.
Can a COVID-19 vaccine give you COVID-19?
No. The COVID-19 vaccines currently being developed in the U.S. don’t use the live virus that causes COVID-19.
Keep in mind that it will take a few weeks for your body to build immunity after getting a COVID-19 vaccination. As a result, it’s possible that you could become infected with the virus that causes COVID-19 just before or after being vaccinated.
What are the possible side effects of a COVID-19 vaccine?
A COVID-19 vaccine can cause mild side effects after the first or second dose, including:
- Pain, redness or swelling where the shot was given
- Fever
- Fatigue
- Headache
- Muscle pain
- Chills
- Joint pain
You’ll likely be monitored for 15 minutes after getting a COVID-19 vaccine to see if you have an immediate reaction. Most reactions happen with the first few days after vaccination and last no more than three days.
If you experience side effects after getting a COVID-19 vaccine, it doesn’t mean that you have COVID-19. Take time to rest and recover. If you develop a fever, stay home. However, it’s not necessary to get a COVID-19 test or quarantine.
If you have a reaction that prevents you from being able to eat, sleep or work, contact your doctor. Also, contact your doctor if you have a reaction that lasts longer than three days.
Signs of an allergic reaction include hives, swelling of the face and throat, difficulty breathing, a fast heartbeat, dizziness, and weakness. If you have any of these signs, seek care immediately.
How are the COVID-19 vaccines being distributed?
Due to limited supplies, not everyone will be able to get a COVID-19 vaccine right away.
The Advisory Committee on Immunization Practices (ACIP) is a U.S. federal advisory group made up of medical and public health experts. The ACIP has recommended that in the first phase of vaccination in the U.S., COVID-19 vaccines should be given to health care personnel and adult residents of long-term care facilities.
The ACIP has also recommended that the next group to get a vaccine in the U.S. should include people age 75 and older and frontline essential workers, such as first responders, teachers and public transit and grocery store workers.
The third priority group recommended to get the vaccine in the U.S. includes people ages 65 to 74, people ages 16 to 64 who are at high risk of severe COVID-19 due to underlying medical conditions and all other essential workers, such as those working in food service and construction. Examples of underlying medical conditions include type 2 diabetes and severe obesity.
Can I get a COVID-19 vaccine if I have a history of severe allergic reactions?
If you have a history of severe allergic reactions not related to vaccines or injectable medications, you may still get a COVID-19 vaccine. You should be monitored for 30 minutes after getting the vaccine.
If you’ve had a severe allergic reaction to other vaccines or injectable medications, ask your doctor if you should get a COVID-19 vaccine. If you’ve ever had a severe allergic reaction to any ingredient in a COVID-19 vaccine, the Centers for Disease Control and Prevention recommends not getting that specific vaccine.
If you have a severe allergic reaction after getting the first dose of a COVID-19 vaccine, don’t get the second dose.
Can pregnant or breastfeeding women get the COVID-19 vaccine?
There is no research on the safety of COVID-19 vaccines in pregnant or breastfeeding women. However, if you are pregnant or breastfeeding and part of a group recommended to get a COVID-19 vaccine, you may choose to get the vaccine. Talk to your health care provider about the risks and benefits.
Is there anyone who should not get a COVID-19 vaccine?
There is no COVID-19 vaccine yet for children under age 16. Several companies have begun enrolling children as young as age 12 in COVID-19 vaccine clinical trials. Studies including younger children will begin soon.
COVID-19 vaccination might not be recommended for people with certain health conditions. Talk to your doctor if you have questions about getting the vaccine.
Should I get the COVID-19 vaccine even if I’ve already had COVID-19?
Getting COVID-19 might offer some natural protection or immunity from reinfection with the virus that causes COVID-19. But it’s not clear how long this protection lasts.
Because reinfection is possible and COVID-19 can cause severe medical complications, it might be recommended that people who have already had COVID-19 get a COVID-19 vaccine. If you’ve had COVID-19, wait until 90 days after your diagnosis to get a COVID-19 vaccine.
Can I stop taking safety precautions after getting a COVID-19 vaccine?
Experts want to learn more about the protection that a COVID-19 vaccine provides and how long immunity lasts before changing safety recommendations. Factors such as how many people get vaccinated and how the virus is spreading in communities will also affect these recommendations.
In the meantime, the Centers for Disease Control and Prevention recommends following these precautions for avoiding infection with the COVID-19 virus:
Avoid close contact. This means avoiding close contact (within about 6 feet, or 2 meters) with anyone who is sick or has symptoms. Also, keep distance between yourself and others. This is especially important if you have a higher risk of serious illness.
Wear cloth face coverings in public places. Cloth face coverings offer extra protection in places such as the grocery store, where it’s difficult to avoid close contact with others. Surgical masks may be used if available. N95 respirators should be reserved for health care providers.
Practice good hygiene. Wash your hands often with soap and water for at least 20 seconds, or use an alcohol-based hand sanitizer that contains at least 60% alcohol. Cover your mouth and nose with your elbow or a tissue when you cough or sneeze. Throw away the used tissue. Avoid touching your eyes, nose and mouth. Avoid sharing dishes, glasses, bedding and other household items if you’re sick. Clean and disinfect high-touch surfaces daily.
Stay home if you’re sick. Stay home from work, school and public areas if you’re sick, unless you’re going to get medical care. Avoid public transportation, taxis and ride-sharing if you’re sick.
If you have a chronic medical condition and may have a higher risk of serious illness, check with your doctor about other ways to protect yourself.