FORBES – Three years ago, Egypt and the United States had approximately the same number of people infected with chronic hepatitis C.
The hepatitis C burden in Egypt was also three to four times higher per capita than in the United States. Today, the situation is very different.
Egypt has been certified by the World Health Organization to be virtually free of the disease. The United States, however, still carries the same burden despite having the resources to eliminate hepatitis C.
Egypt’s 100 Million Healthy Lives program achieved country wide elimination by demonstrating the will and organization to do so, as well as finding a way to cover the costs. Unfortunately, the United States seems to lack those same tenets.
Recently, the current administration took a major step forward and laid out a historic $11 billion plan to eliminate hepatitis C in the United States within five years.
“40% of the United States’ population is unaware of their [hepatitis C] infection status until severe, often irreversible liver damage occurs.”
The $11 Billion Dollar Plan
The barriers that the United States faces to eliminate hepatitis C are comparable to the barriers that Egypt faced.
The United States must also demonstrate a strong will to eliminate the disease, organize its infrastructure and resources, and find ways to lower the high costs of diagnostics and drugs.
The success of Egypt’s 100 Million Healthy Lives campaign provided an excellent model for creating a hepatitis elimination plan, and in March of this year, the current administration revealed its Nation Hepatitis Elimination Program.
Outlined in the government budget for fiscal year 2024, this five year and $11.3 billion plan is a declaration of the United States’ willingness to eliminate hepatitis C.
It establishes a cohesive effort that brings together all facets of the healthcare delivery system including state governments, federal agencies, and community health providers.
The National Hepatitis Elimination Program plan outlines four main objectives that aim to “increase access to curative medications and expand implementation of complementary efforts such as screening, testing, and provider capacity.”
These objectives are designed to tackle all three of the main elimination barriers: the will, the organization, and the cost … READ MORE.
Mayo Clinic News Network: Treating hepatitis C
By Liza Torborg, January 22, 2019
Receiving a diagnosis of hepatitis C can be distressing. The infection poses a risk of liver damage and, although rare, it may lead to liver cancer. Fortunately, thanks to recent advances in treatment, highly effective antiviral medication is available to treat hepatitis C. At this point, you should consult with a physician who specializes in liver diseases to help you decide how best to proceed with your care.
Hepatitis C is a viral infection that causes liver inflammation. It is spread through contact with blood that’s infected with the virus. Numerous factors have been associated with an increased risk for this infection, such as receiving a blood transfusion or organ transplant before 1992, injection of illicit drugs, and receiving a tattoo or piercing with equipment that is contaminated. People born between 1945 and 1965 have the highest rate of hepatitis C infection, and they should be tested for the virus.
Most individuals diagnosed with hepatitis C have had it for years without noticing any symptoms. The virus doesn’t trigger symptoms until it’s started to damage the liver.
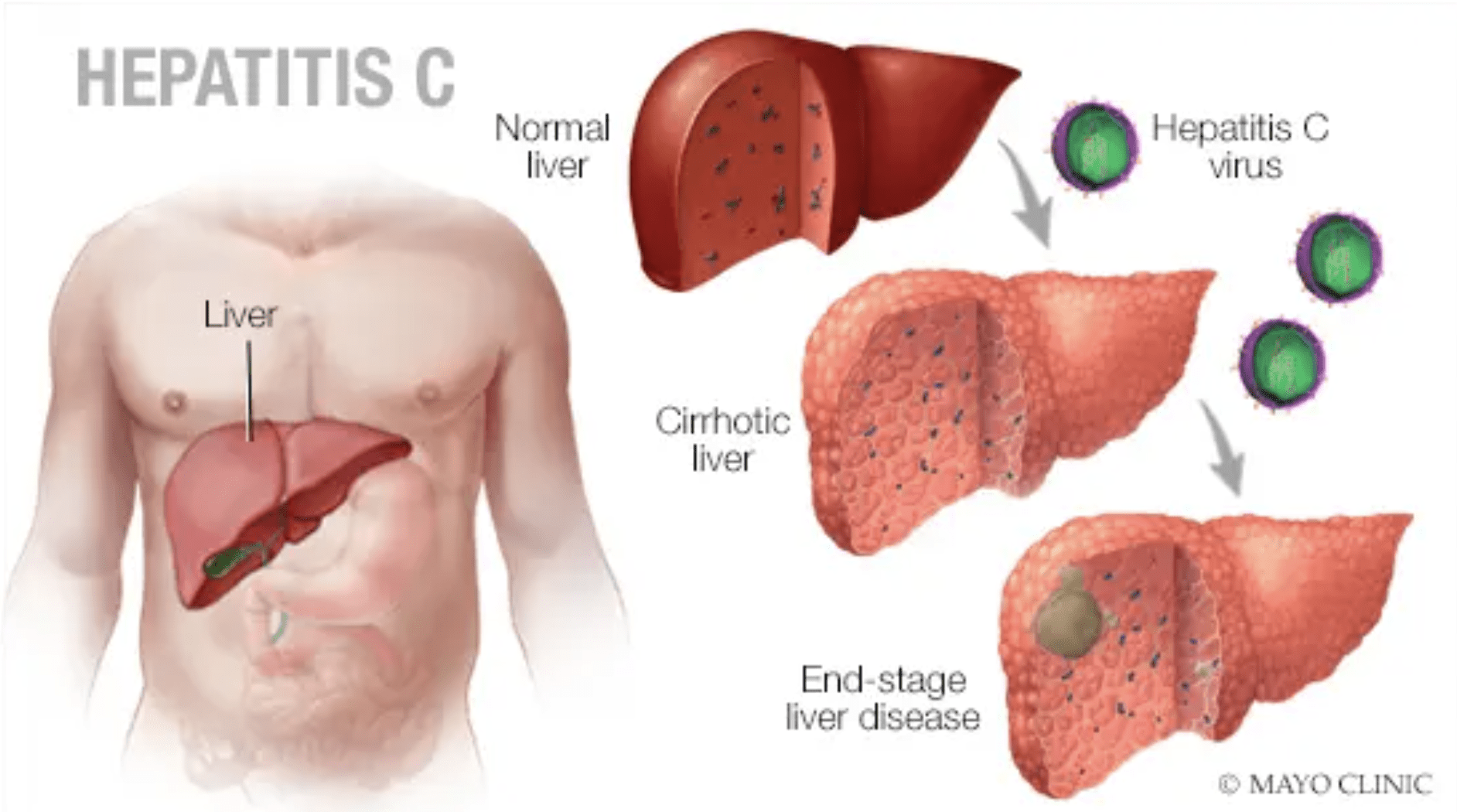
Progressive liver damage in the form of extensive fibrosis, or liver scarring, called “cirrhosis,” occurs in about 25 percent of people with hepatitis C.
The risk of cirrhosis in people infected with the hepatitis C virus is higher among those who are obese and drink heavy amounts of alcohol. An occasional alcoholic drink is not thought to increase the risk of cirrhosis significantly.
Individuals who develop cirrhosis as a result of hepatitis C have a 2 to 3 percent annual risk of developing primary liver cancer. Those with a lesser degree of liver fibrosis typically are not at increased risk for developing liver cancer.
Even without the development of liver cancer, however, if hepatitis C is left untreated, liver damage may progress to the point that it causes loss of liver function. Eventually, that could lead to a liver transplant in a small percentage of patients.
Because it’s difficult to predict who will develop serious liver damage from hepatitis C, antiviral treatment is recommended for everyone diagnosed with the virus. The antiviral medication used to fight hepatitis C is effective in eradicating the virus. By taking a single pill once a day for eight to 12 weeks, a patient has a greater than 95 percent chance of being cured permanently.
Clearing the hepatitis C virus from the body halts the progression of liver fibrosis and leads to regression of fibrosis in most cases. Side effects from the medication, when they happen at all, are minimal.
The next step for you is to ask your health care provider for a referral to a specialist in liver diseases. He or she can conduct an examination and recommend tests to evaluate your liver function and assess your degree of liver fibrosis. How quickly you’ll need to begin antiviral treatment depends on the results of that assessment. — Dr. John Gross, Gastroenterology, Mayo Clinic, Rochester, Minnesota | SOURCE