Jun 3, 2020
Jun 3, 2020
Best Life – Your nose may help keep you safe from COVID-19. If you ever enter a room or building and pick up a musty smell, it just may be a good indicator that the space is high risk for coronavirus.
Amid COVID-19, “areas that seem musty, stale, stuffy, or any other sign that the air is not moving” should be avoided, Bruce Y. Lee, professor of Health Policy and Management at the City University of New York School of Public Health, wrote for Forbes. “That applies to bars, restaurants, stores, and other business establishments, too.”
Why is that? Well, that musty stench could be the sign of poor ventilation.
“Poor ventilation can be an assault on the senses, including smell. In a home or room where the moisture can’t escape, it can develop a musty smell,” according to the experts at heating, cooling, and ventilation company HRV.
This means if you can easily pick up the scent of mold, mildew, rot, or dampness, you may be entering a space that has poor ventilation. And because coronavirus can be transmitted through contagious respiratory droplets that hang in the air, proper ventilation is pivotal in removing those pathogens from the air you breathe indoors … Read more.
RECENTLY:
If This Sense Fails, You May Have Coronavirus
A Grim Reality of Reopening: Unhealthy Mold
Which test is best for COVID-19?
Sep 21, 2020, Robert H. Shmerling, MD, Senior Faculty Editor
Harvard Health Publishing – Now that we’re several months into the COVID-19 pandemic, steps we need to take to effectively control the outbreak have become clear: conscientious prevention measures like handwashing and distancing, widespread testing with quick turnaround times, and contact tracing.
None of these is easy to maintain over a prolonged period. But combined, they are our best bets while awaiting better treatments and an effective vaccine.
So, which tests to use?
The many types of tests available are sowing considerable confusion. Unfortunately, because this novel coronavirus is indeed novel, and COVID-19 is a new disease, information about these tests is incomplete and the options for testing keep changing.
But here’s what we know now about tests designed to diagnose a current infection, and those that show whether you previously had the virus.
Diagnostic tests for current infection
If you want to know if you are currently infected with the COVID-19 virus, there are two types of tests: molecular tests and antigen testing.
Molecular tests (also called PCR tests, viral RNA tests, nucleic acid tests)
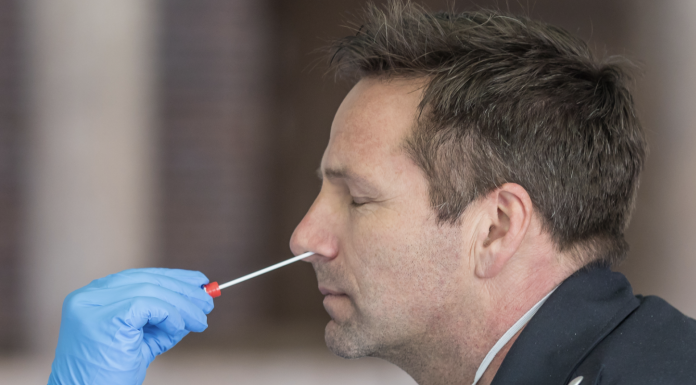
How is it done? Nasal swabs, throat swabs, and tests of saliva or other bodily fluids.
Where can you get this test? At a hospital, in a medical office, in your car, or even at home.
What does the test look for? Molecular tests look for genetic material that comes only from the virus.
How long does it take to get results? It depends on lab capacity. Results may be ready the same day, but usually take at least a day or two. Throughout the pandemic, especially lately, delayed turnaround times of up to a week or two have been reported in many places.
What about accuracy? False negatives — that is, a test that says you don’t have the virus when you actually do have the virus — may occur. The reported rate of false negatives is as low as 2% and as high as 37%. The false positive rate — that is, how often the test says you have the virus when you actually do not — should be close to zero. Most false-positive results are thought to be due to lab contamination or other problems with how the lab has performed the test, not limitations of the test itself.
A molecular test using a deep nasal swab is usually the best option, because it will have fewer false negative results than other diagnostic tests or samples from throat swabs or saliva. People who are in the hospital, though, may have other types of samples taken.
You may have heard about pooled testing, in which multiple samples are combined and a molecular test is performed on them. This could speed up the testing of large numbers of people and reduce the number of tests needed.
If a pooled test is negative, the people whose samples were combined are told they have a negative test and individual testing is unnecessary. But if the pooled sample tests positive, each of the individual samples that were taken will then be tested to see which person(s) is responsible for the positive pooled result.
This approach may be particularly helpful in settings where the number of infections is low and declining, and most test results are expected to be negative.
For example, in a community where the infection seems to be under control and reopenings of schools and businesses are planned, pooled testing of employees and students could be an effective strategy.
Antigen tests
How is it done? A nasal or throat swab.
Where can you get these tests? At a hospital or doctor’s office (though it is likely home testing will soon be available).
What does the test look for? This test identifies protein fragments (antigens) from the virus.
How long does it take to get results? The technology involved is similar to a pregnancy test or a rapid strep test, with results available in minutes … Read more.