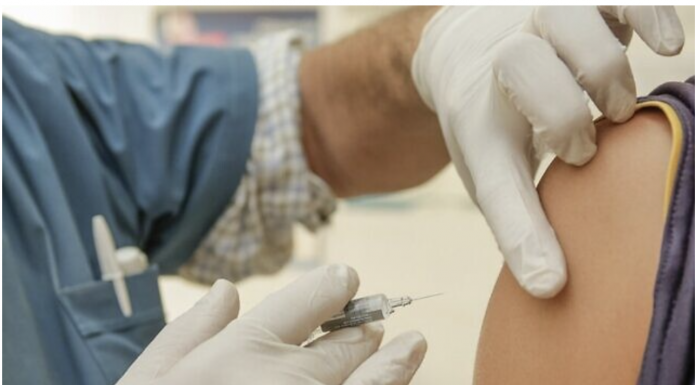
Myths and fears: Rumors have been circulating that the vaccine is designed to control or eliminate certain groups within our society, to allow for “mind control” of vaccinated people, or to allow certain “elite” members of society to rule the rest of us.
The bottom line: All of these are false. The vaccine will be available to everyone in the United States, in an order that’s determined by two things: each person’s risk of being exposed to COVID-19 at work or where they live, and their risk of getting seriously ill or dying from COVID-19 because of their age and underlying health conditions.
More detail: Studies have shown that people who are older or have certain medical conditions – including being overweight or obese, and smoking – are more likely to get seriously ill if they catch the coronavirus. The more virus a person is exposed to, and the more often they’re exposed, the higher their chance of getting sick. Exposures can happen at work or at home, especially when many people live together.
FACT: The COVID-19 vaccine can end the pandemic much sooner, and with fewer lives lost. This could especially help people in the highest risk groups, including people of color.
Studies of COVID-19 patterns have shown that people in certain groups – Black, Native American and Latino people, for example – have a higher risk of severe or fatal COVID-19 than people in other groups. This is probably due to multiple factors including group-level differences in health, type of employment, living situation and access to health care.
But priority order for vaccination is based on the individual’s own personal risk, not the group they belong to, their skin color, what languages they speak at home, their income or their education level.
For instance, a healthy person in their 30s who works from home via the internet will be further back in the vaccine line than an older, heavier person with diabetes who works in a hardware store. Meanwhile, a pregnant woman working in a grocery store would be behind an 80-year-old who lives in a nursing home, but ahead of a healthy middle-aged person who farms with their family.
It is understandable that some people may be more likely to mistrust the COVID-19 vaccine because of discrimination against people like them in other aspects of modern life or history. Our country also has an unequal distribution of access to health care, preventive health services and health education.
Every person must decide what they will do, but they should consider both their personal risks of COVID-19 and the benefits of vaccines in reducing that risk for themselves and society
FACT: The coronavirus is changing. But vaccines are designed to help the body recognize it based on multiple parts of the virus.
Myths and fears: New mutations in the coronavirus have been reported, which may change the exact nature of the proteins on its surface. This has led to fears that the vaccines developed so far might not work against these new “mutants” because vaccines are based on teaching the body to recognize those proteins and attack them in future.
The bottom line: So far, COVID-19 vaccine makers say that the new mutations seen in the novel coronavirus have not “outsmarted” the vaccines.
Many harmful viruses can change over time as they hijack our cells (or the cells of animals) and fool them into making more copies of the virus that we can then transmit to other people or animals. This is why we have to have a new flu vaccine every year, to fine-tune it to the strains of influenza virus that are circulating.
The vaccines teach the body about multiple “spike” proteins on the virus surface, and those spikes are also what the virus uses to get inside our cells. So a change in one protein because of a mutation doesn’t automatically make the whole vaccine useless.
But it’s important for scientists to keep looking for mutations in the coronavirus that’s infecting people now. This will help them know if we need to change the current vaccines or make new vaccines against COVID-19.
Meanwhile, scientists are still studying whether changes in the coronavirus are making it more likely to spread, more likely to infect children and teenagers, or more likely to cause serious illness or death. It will take time to find all these things out. That’s why it’s important to continue to wear masks in public, and stay away from large gatherings and unmasked interactions with people who don’t live with you.
FACT: People who have health conditions that affect their immune system, or have gotten treatments that reduce their immune response, should talk to their doctor about vaccination.
Myths and fears: People who have autoimmune disorders such as rheumatoid arthritis or lupus, or who have received treatments that change their immune response, such as bone marrow transplants, chemotherapy, steroids or drugs that work against HIV, may be worried that they could react to the vaccine, or not get protected by it.
The bottom line: People with these conditions were generally not included in the clinical trials of COVID-19 vaccines, so we don’t have strong information about how much of an immune response the vaccine will produce in them.
Depending on your individual risk of getting exposed to coronavirus, and your precise condition or treatment, you and your doctor should discuss whether or not to get vaccinated when it’s your turn.
The CDC maintains a list of health conditions that are, or might be, associated with a higher risk of severe COVID-19. People with these conditions who are not frontline health care workers, nursing home residents or workers in essential or critical jobs, are likely to be prioritized for vaccination, but specific recommendations have not been made yet.
TO BE CONTINUED …
(c) Michigan Medicine, Creative Commons Attribution 3.0 license.
PREVIOUSLY IN THIS SERIES:
Part I: “Corners Were Cut In Covid Vaccine Testing”: TRUE or FALSE?
Part II: “The Vaccine Changes Your DNA”: TRUE or FALSE?
Part III: “People Are Getting Seriously Ill From Vaccines”: TRUE or FALSE?