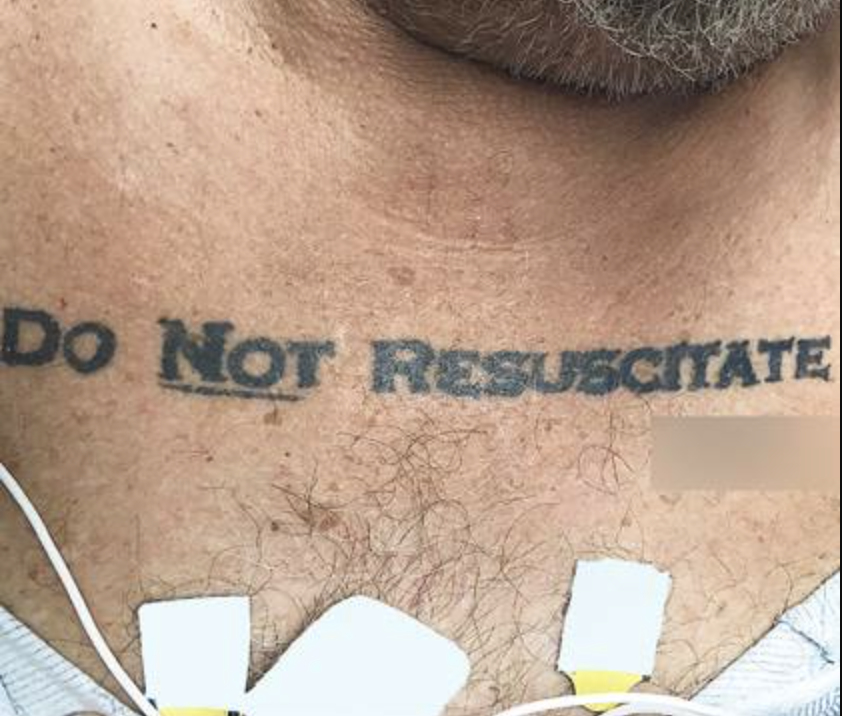
MAYO CLINIC NEWS NETWORK – With the growing popularity of tattoos, you may wonder if a tattoo is the best way to express health care wishes. Tattooing “DNR” or “DNI” on your chest may seem like an easy way to permanently express your wishes. But this is ethically controversial and not a substitute for a valid advance directive.
In Wisconsin and Minnesota, a tattoo is not acceptable by law for expressing end-of-life care wishes. This is because it doesn’t include the information required, such as your name, address and phone number. It also doesn’t have the signature of your attending physician. Finally, a tattoo is not easily reversible.
Do not resuscitate (DNR) and do not intubate (DNI) tells your health care team that you do not want to be resuscitated or have intubation in an emergency. Resuscitation refers to cardiopulmonary resuscitation, also called CPR. This treatment tries to restart a normal heartbeat if it stops beating or beats very irregularly by pushing on the chest forcefully, called chest compressions. Intubation refers to placing a plastic tube down a person’s breathing tube and placing them on life support breathing machines or ventilators.
It might be difficult to understand why anyone would not want all measures to be taken to save a life. Generally, a person who has terminal illness or a history of chronic disease may prefer a natural death without heroic measures to try and bring he or she back to life. Lifesaving measures often do not bring a person back to the previous level of function, usually cause broken ribs and can cause disability or lead to an unpleasant death.
Ultimately, your health care team won’t know of your wishes unless you record them in an advance directive and have it added to your medical record. Do not rely on a tattoo to communicate this important information.
Who should complete an advance directive?
Every person, 18 and older, should complete an advance directive. In Wisconsin or Minnesota, if you are too sick to say what you want and do not have an advance directive on file, a judge might appoint a guardian to make medical decisions for you. It’s important that you write down what you think is best for you and not what others would want for you. This document is a gift to your loved ones.
Just as important as an advance directive is the conversation with family and friends. Some people fear that speaking to their loved ones about their final days would be too grim. In reality, these are among the most empowering and meaningful conversations people can have.
The decisions you make should align with your values. What is most important to you, and what gives your life meaning? What are your preferences for health care? And, just as important, what are your limits?
It’s critical to know that emergency responders cannot follow advance directives in emergency situations.
If you wish to avoid aggressive treatment in an ambulance, emergency responders can honor your wishes, but only if you have a Physician Order for Scope of Treatment or are wearing a state-approved community do-not-resuscitate bracelet. Talk with your health care team if you wish to have a do-not-resuscitate bracelet or would like to discuss advance care planning and complete these documents.
Hilary Bingol, M.D., is the director of Hospice and chair of Palliative Medicine in La Crosse, Wisconsin.