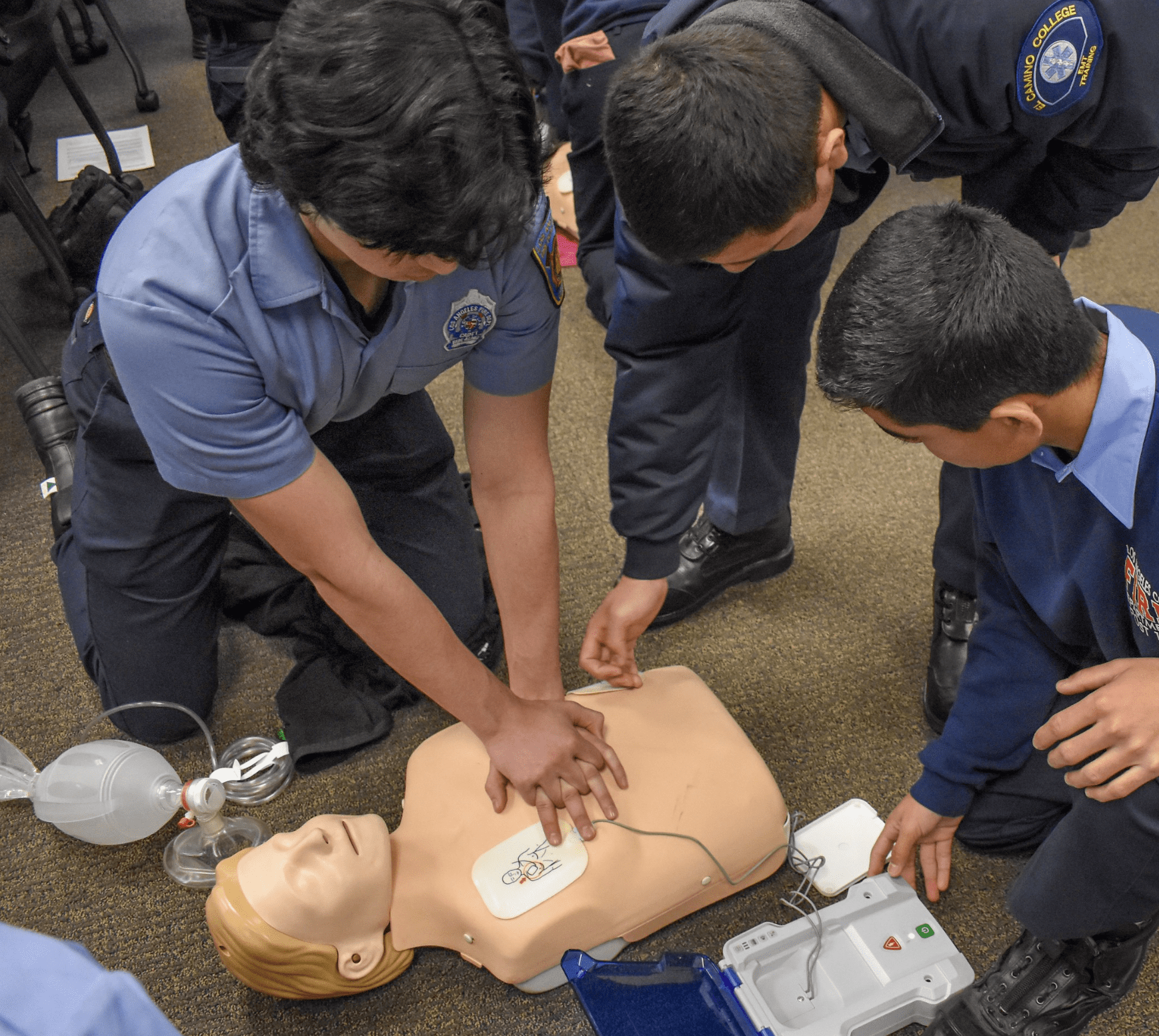
NPR – “Nurse refuses to perform CPR,” read the caption on an ABC newscast in California. “911 dispatcher’s pleas ignored.”
Several days earlier, an elderly woman at a senior living facility had gone into cardiac arrest. The dispatcher instructed an employee to perform CPR, or cardiopulmonary resuscitation. But the employee refused.
“Is there anybody there that’s willing to help this lady and not let her die?” the dispatcher said. It made the local news, which elicited a national outcry and prompted a police investigation.
But the woman was already dead — her heart had stopped. And according to family, the woman had wished to “die naturally and without any kind of life-prolonging intervention.”
So why the controversy? It comes down to a widespread misconception of what CPR can, and can’t, do. CPR can sometimes save lives, but it also has a dark side.
In the 1970s, CPR classes were developed for the public, and CPR became the default treatment for cardiac arrest. Flight attendants, coaches, and babysitters are now often required to be certified.
Many people learn what they know about CPR from television. In 2015, researchers found that survival after CPR on TV was 70%. In real life, people similarly believe that survival after CPR is over 75%.
Those sound like good odds, and this may explain the attitude that everyone should know CPR, and that everyone who experiences cardiac arrest should receive it.
Two bioethicists observed in 2017 that “CPR has acquired a reputation and aura of almost mythic proportions,” such that withholding it might appear “equivalent to refusing to extend a rope to someone drowning.”
But the true odds are grim. In 2010 a review of 79 studies, involving almost 150,000 patients, found that the overall rate of survival from out-of-hospital cardiac arrest had barely changed in thirty years. It was 7.6% …
Clayton Dalton is a writer in New Mexico, where he works as an emergency physician.